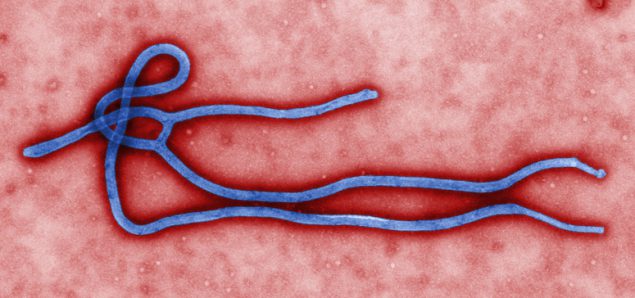
The U.S. Food and Drug Administration approved Inmazeb (atoltivimab, maftivimab, and odesivimab-ebgn), a mixture of three monoclonal antibodies, as the first FDA-approved treatment for Zaire ebolavirus (Ebola virus) infection in adult and pediatric patients.
Zaire ebolavirus, commonly known as Ebola virus, is one of four Ebolavirus species that can cause a potentially fatal human disease. Ebola virus is transmitted through direct contact with blood, body fluids and tissues of infected people or wild animals, as well as with surfaces and materials, such as bedding and clothing, contaminated with these fluids. Individuals who provide care for people with Ebola virus, including health care workers who do not use correct infection control precautions, are at the highest risk for infection.
Inmazeb targets the glycoprotein that is on the surface of Ebola virus. Glycoprotein attaches to the cell receptor and fuses the viral and host cell membranes allowing the virus to enter the cell. The three antibodies that make up Inmazeb can bind to this glycoprotein simultaneously and block attachment and entry of the virus.
Inmazeb was evaluated in 382 adult and pediatric patients with confirmed Zaire ebolavirus infection in one clinical trial (the PALM trial) and as part of an expanded access program conducted in the Democratic Republic of the Congo (DRC) during an Ebola virus outbreak in 2018-2019. The PALM trial was led by the U.S. National Institutes of Health and the DRC’s Institut National de Recherche Biomédicale with contributions from several other international organizations and agencies.
In the PALM trial, the safety and efficacy of Inmazeb was evaluated in a multi-center, open-label, randomized controlled trial, in which 154 patients received Inmazeb (50 mg of each monoclonal antibody) intravenously as a single infusion, and 168 patients received an investigational control. The primary efficacy endpoint was 28-day mortality. The primary analysis population was all patients who were randomized and concurrently eligible to receive either Inmazeb or the investigational control during the same time period of the trial. Of the 154 patients who received Inmazeb, 33.8% died after 28 days, compared to 51% of the 153 patients who received a control. In the expanded access program, an additional 228 patients received Inmazeb.
The most common symptoms experienced while receiving Inmazeb included: fever, chills, tachycardia (fast heart rate), tachypnea (fast breathing), and vomiting; however, these are also common symptoms of Ebola virus infection. Patients who receive Inmazeb should avoid the concurrent administration of a live vaccine due to the treatment’s potential to inhibit replication of a live vaccine virus indicated for prevention of Ebola virus infection and possibly reduce the vaccine’s efficacy.
Hypersensitivity, including infusion-related events, can occur in patients taking Inmazeb, and treatment should be discontinued in the event of a hypersensitivity reaction.
Inmazeb received an Orphan Drug designation for the treatment of Ebola virus infection. The Orphan Drug designation provides incentives to assist and encourage drug development for rare diseases. Additionally, the agency granted Inmazeb a Breakthrough Therapy designation for the treatment of Zaire ebolavirus infection.
The FDA is granting the approval to Regeneron Pharmaceuticals.
The FDA approved Ervebo, the first vaccine for the prevention of Ebola virus disease, in December 2019, with support from a study conducted in Guinea during the 2014-2016 Ebola outbreak.
The FDA, an agency within the U.S. Department of Health and Human Services, protects the public health by assuring the safety, effectiveness, and security of human and veterinary drugs, vaccines and other biological products for human use, and medical devices. The agency also is responsible for the safety and security of our nation’s food supply, cosmetics, dietary supplements, products that give off electronic radiation, and for regulating tobacco products.